Thyroid nodules occur in 50% of the population now. Hence, radiofrequency ablation for thyroid treatment becomes popular now. Although most thyroid nodules do not cause symptoms and are often discovered incidentally to other medical conditions, some individuals experience problems such as swallowing difficulties, neck pain, or having a cosmetic concerns due to nodule size.
Traditionally, surgery was the primary treatment to address large and symptomatic nodules. However, radiofrequency ablation (RFA) has now become a revolutionary non-surgical treatment that provides similar relief, affords reliability, and is free of surgical risks.
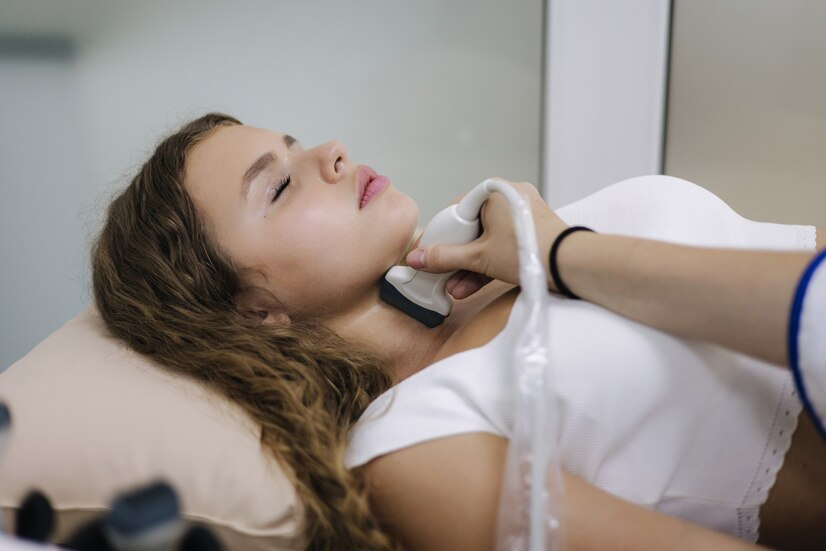
What is Radiofrequency Ablation (RFA)?
Radiofrequency Ablation for Thyroid Nodules is a minimally invasive procedure that uses thermal energy to shrink or destroy targeted tissue. For those suffering from thyroid nodules, this means a way to alleviate symptoms without the scarring, long recovery, and possible hormonal imbalances often associated with traditional thyroid surgery.
How Does RFA Work?
- Step 1: Preparation
Patients are prepped with local anesthesia to ensure minimal discomfort. Ultrasound imaging is used to visualize the nodule clearly. - Step 2: Precision Ablation
An experienced specialist inserts a thin, needle-like probe directly into the thyroid nodule. The probe delivers high-frequency electrical currents, which generate heat and target the nodule cells precisely. - Step 3: Natural Absorption
The heat effectively destroys the abnormal thyroid tissue, which the body then gradually absorbs. Over time, this results in a notable decrease in nodule size.
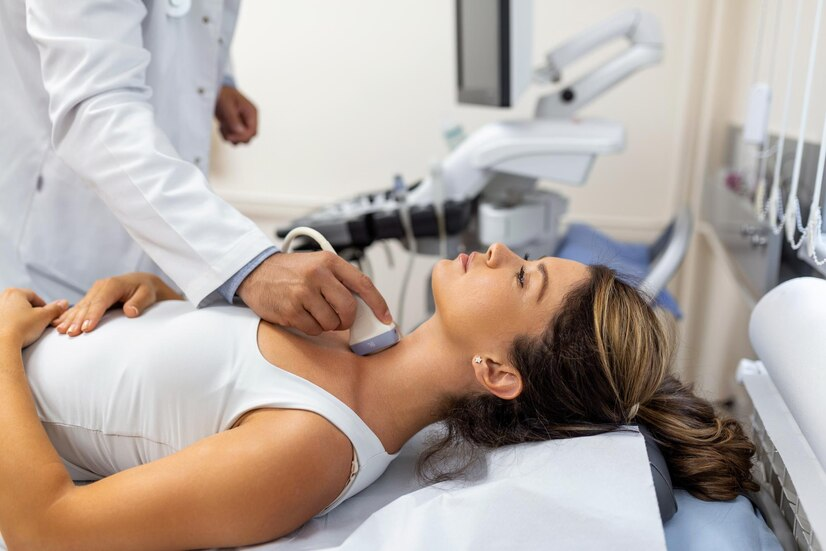
The Science Behind Radiofrequency Ablation for Thyroid Nodules
Radiofrequency Ablation for Thyroid Nodules foundation lies in the principle of thermal ablation. The high-frequency electrical energy transforms into heat, causing cellular destruction. Once the damaged tissue is broken down, the body naturally clears it away, leaving a significantly smaller nodule. But why has RFA gained so much attention, particularly in thyroid treatment?
Effectiveness Backed by Research
- A comprehensive study in the American Journal of Endocrinology (2022) showed that RFA reduces nodule size by 60-85% within six months.
- Another investigation demonstrated that over 90% of patients report symptom relief, including the reduction of pressure in the neck and improved cosmetic appearance.
These outcomes make RFA a standout alternative, especially for patients who are hesitant about surgery or hormone replacement therapy.
Why Choose Radiofrequency Ablation for Thyroid Nodules Over Surgery?
While thyroid surgery, or thyroidectomy, has long been the gold standard for treating large or symptomatic nodules, RFA offers unique advantages that make it increasingly popular.
1. Non-Surgical and Scar-Free
One of the most appealing features of Radiofrequency Ablation for Thyroid Nodules is that it leaves no scar. The procedure is performed using a fine needle, unlike surgery, which requires a neck incision. For those concerned about aesthetics, this is a significant benefit.
2. Shorter Recovery Time
Post-surgical recovery can take several weeks, often accompanied by pain, dietary restrictions, and the inability to perform daily activities. In contrast, RFA patients typically return to work and routine life within one to two days. The procedure itself is usually completed in under an hour.
3. Thyroid Function Preservation
Surgery often involves removing all or part of the thyroid gland, leading to potential hormone imbalances and lifelong dependence on thyroid hormone replacement. RFA, on the other hand, focuses only on the nodule, preserving the overall gland and its function.
4. Reduced Risk of Complications
Though any medical intervention comes with risks, RFA has a lower complication rate compared to surgery. This is particularly significant for patients with underlying health issues that make them poor candidates for general anesthesia.
Who Should Consider Radiofrequency Ablation for Thyroid Nodules?
RFA isn’t for everyone, but it offers an excellent solution for many patients with benign thyroid nodules. Let’s delve into the specifics:
Ideal Candidates
- Confirmed Benign Nodules: Before undergoing RFA, a fine-needle aspiration biopsy must confirm that the nodule is non-cancerous.
- Symptomatic Nodules: Those causing discomfort, difficulty swallowing, or cosmetic concerns are ideal candidates.
- Desire to Avoid Surgery: Patients who prefer to keep their thyroid intact and avoid the risks of surgical intervention are likely to benefit.
Who Might Not Be Eligible?
- Very Large Nodules: While RFA is effective, extremely large or calcified nodules may not shrink adequately.
- Complex Thyroid Cases: Patients with malignant or suspicious nodules, or those with multiple complicated thyroid conditions, should explore other options
How Radiofrequency Ablation for Thyroid Nodules Is Performed: Step-by-Step Guide
To fully appreciate the effectiveness and convenience of Radiofrequency Ablation for thyroid nodules, understanding the detailed procedure is essential. Here is a breakdown:
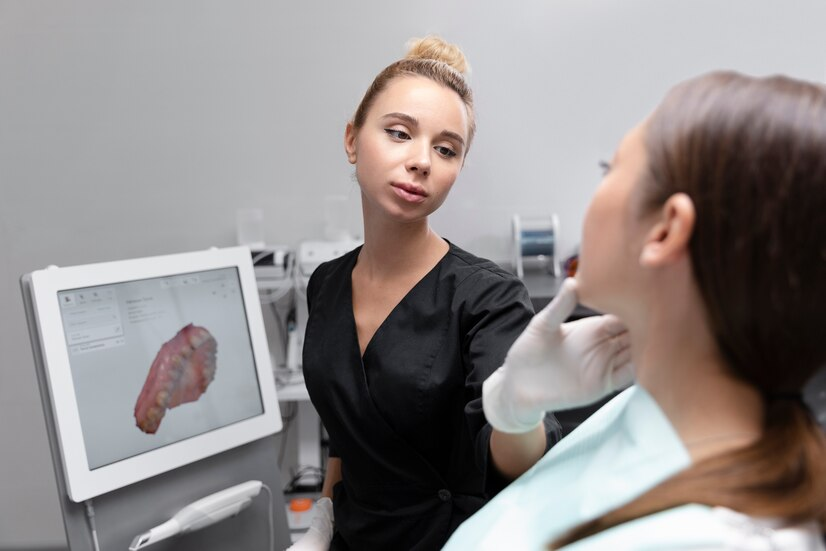
- Pre-Procedure Assessment
- Before RFA, patients undergo comprehensive screening, including ultrasound imaging and a fine-needle aspiration biopsy, to confirm the benign nature of the thyroid nodule.
- The medical team evaluates the size, location, and characteristics of the nodule to customize the treatment approach.
- Preparation and Anesthesia
- RFA is performed under local anesthesia, which numbs the area around the thyroid. This ensures patient comfort and minimal discomfort during the procedure.
- Real-time ultrasound guidance is crucial. It allows the specialist to precisely place the RFA probe and monitor the nodule throughout the treatment.
- Insertion of the RFA Probe
- A thin, needle-like probe is carefully inserted into the thyroid nodule. The probe’s placement is adjusted as necessary to ensure maximum efficacy while protecting surrounding tissues.
- Delivery of Thermal Energy
- High-frequency electrical currents pass through the probe, generating heat that destroys the nodule cells. This process is meticulously controlled to avoid affecting healthy thyroid tissue or surrounding structures like the vocal cords and blood vessels.
- The heat induces necrosis (cell death) in the nodule tissue, which the body will naturally absorb over time.
- Post-Procedure Care
- The entire procedure usually takes between 30 to 60 minutes. Patients are monitored for a short period afterward to ensure there are no immediate complications.
- Most patients report little to no pain and can return to normal activities within 24 to 48 hours. The use of over-the-counter pain relief is typically sufficient for any minor post-procedural discomfort.
The Cost of RFA: Is It Worth It?
The financial aspect of medical treatments is a significant consideration. So, how does RFA stack up in terms of cost-effectiveness compared to traditional surgery?
- Understanding the Price Range
- The cost of RFA for thyroid nodules varies widely based on factors like geographical location, the healthcare provider, and the complexity of the case. On average, it ranges from $3,000 to $10,000 per session.
- While this may seem steep, RFA is often less expensive than traditional thyroidectomy, especially when factoring in the costs associated with extended hospital stays, anesthesia, and post-surgical care.
- Insurance Coverage: What to Know
- Insurance coverage for RFA is an evolving area. Some insurers cover the procedure if it is deemed medically necessary, while others may still consider it experimental. Patients are advised to consult with their healthcare provider and insurance company to understand their coverage options.
- Cost comparisons also highlight that even if RFA has a higher out-of-pocket expense initially, it may still be more economical in the long run, particularly if the patient avoids lifelong thyroid hormone replacement therapy.
Effectiveness and Long-Term Outcomes
One of the most important questions patients have about RFA is, “How effective is it, really?” Let’s look at the long-term success stories and the compelling data behind them.
- Success Rates and Shrinkage Metrics
- Studies consistently show that RFA can reduce nodule volume by 60-85% within the first six months.
The reduction continues over a year, with many patients experiencing nearly 90% shrinkage of the nodule. - A multicenter trial conducted in 2021, involving over 1,000 patients, found that symptom relief was sustained even three years post-treatment, showcasing the procedure’s enduring efficacy.
- Studies consistently show that RFA can reduce nodule volume by 60-85% within the first six months.
- Symptom Relief and Quality of Life
- Patients frequently report significant improvements in symptoms, including alleviated pressure on the neck, better swallowing, and an enhanced cosmetic appearance.
- Psychological well-being also benefits. Many individuals feel a sense of relief and increased confidence once their physical symptoms and neck appearance improve.
- Risk and Recurrence Factors
- Although highly effective, RFA is not entirely risk-free. Some potential complications include temporary voice changes, minor bleeding, or transient swelling. However, these are relatively rare, occurring in less than 1% of cases.
- Recurrence of nodules is another consideration. Research indicates that the risk of regrowth is low, especially when patients adhere to follow-up appointments and monitoring.
RFA vs. Alternative Treatments
To understand why RFA is becoming a preferred choice, it’s helpful to compare it with other treatments for thyroid nodules.
- Traditional Thyroid Surgery
- Pros: Surgery is effective for large or malignant nodules and offers a permanent solution. It’s a tried-and-true method that has been refined over decades.
- Cons: The risks include potential damage to the vocal cords, a lifelong need for thyroid hormone replacement, and visible neck scars. Recovery can be lengthy and painful.
- Ethanol Ablation
- Pros: Another minimally invasive option, often used for cystic thyroid nodules. It involves injecting ethanol into the nodule to induce cell death.
- Cons: It is less effective than RFA for solid nodules and carries a higher risk of recurrence.
- Laser Ablation
- Pros: Similar to RFA in being minimally invasive, using heat to reduce nodule size.
- Cons: Laser ablation is less widely studied and may not be as effective or versatile as RFA for larger or more complex nodules.
Advantages of Radiofrequency Ablation Over Traditional Methods
RFA’s benefits are numerous and have led to its growing popularity as a leading treatment for benign thyroid nodules.
- Minimally Invasive Nature
- Unlike traditional surgery, RFA is performed through a tiny incision, usually no more than a few millimeters wide. This leads to a significantly shorter recovery period and minimal scarring. Most patients return to their daily routines within days rather than weeks.
- Furthermore, the localized nature of the procedure means that general anesthesia is not required, reducing risks associated with anesthesia, particularly in older or medically vulnerable patients.
- Preservation of Thyroid Function
- A critical advantage of RFA is that it spares healthy thyroid tissue. While surgical thyroidectomy often necessitates lifelong hormone replacement therapy, RFA preserves thyroid functionality in nearly all cases.
- This preservation is a significant benefit for younger patients or those who are averse to lifelong medication.
- Fewer Complications and Risks
- RFA has a remarkably low complication rate, typically under 1%, compared to traditional surgery, where risks such as damage to the recurrent laryngeal nerve and hypoparathyroidism are more common.
- The minimal invasiveness of RFA also means reduced risk of infection and post-surgical complications like hematomas.
- Cosmetic Benefits
- For many patients, the appearance of a neck scar from surgery can be distressing. RFA, however, results in virtually no visible scars, which is a significant cosmetic advantage, especially for younger individuals.
What the Future Holds: Advancements in RFA Technology
The field of thyroid nodule treatment continues to evolve, with several promising advancements in RFA technology on the horizon.
- Innovations in Probe Design
- Recent research has focused on developing more advanced RFA probes that provide better energy distribution and more uniform tissue ablation. These innovations aim to improve treatment outcomes and minimize the risk of incomplete nodule destruction.
- Another advancement is the use of multi-electrode RFA systems, which can treat larger nodules more efficiently, further enhancing the procedure’s safety and efficacy.
- Combination Treatments
- Some studies are exploring the potential of combining RFA with other therapies, such as ethanol ablation or medication, to maximize nodule reduction. This approach may be especially beneficial for patients with nodules that are resistant to standard RFA.
- AI and Imaging Technology
- The integration of artificial intelligence (AI) into ultrasound imaging is another exciting development. AI-driven ultrasound can help practitioners achieve more precise probe placement and better assess the nodule’s response to treatment in real time.
Conclusion
From a medical perspective, RFA has transformed the way benign thyroid nodules are treated. Doctors like that it delivers lasting symptom relief significantly shrinks nodules, and allows patients to get back to their lives almost immediately. And unlike surgery, there’s no need for general anesthesia, no scarring, and no lengthy recovery. It’s a win-win for patients and physicians alike.
So, what’s the takeaway? If you’re looking for a safe, efficient, and life-changing approach to managing thyroid nodules, doctors agree: Radiofrequency Ablation for Thyroid Nodules might just be the future you’ve been waiting for. Of course, a thorough evaluation is key, so partner with an experienced thyroid specialist to see if this cutting-edge treatment is your perfect match.
FAQs
1. Is RFA suitable for all types of thyroid nodules?
RFA is primarily indicated for benign thyroid nodules that cause symptoms or cosmetic concerns. It is not suitable for malignant nodules or those with suspicious biopsy results.
2. How long do the effects of RFA last?
Long-term studies show sustained nodule shrinkage and symptom relief for up to five years post-treatment. However, ongoing ultrasound monitoring is crucial to catch any potential regrowth early.
3. Can RFA be repeated if necessary?
Yes, RFA can be safely repeated if the nodule does not shrink adequately or if new nodules develop. The procedure’s repeatability is a key advantage over more invasive surgical options.
4. What are the most common side effects?
Minor side effects include temporary pain, swelling, or voice changes, which typically resolve within a few weeks. Serious complications are exceedingly rare.
5. How does RFA compare with other non-surgical treatments?
Compared to ethanol ablation or laser ablation, RFA is more versatile and effective for larger, solid nodules. The choice of treatment should always be based on a thorough discussion between the patient and their healthcare provider.
